Eczema In Children
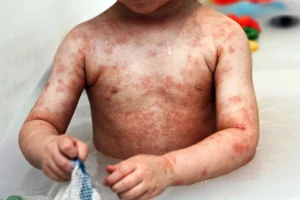
Eczema in Children: A Comprehensive Guide to Atopic Dermatitis from Infancy to Adolescence
Introduction: The Itch That Rashes
Eczema, clinically known as atopic dermatitis, is more than just a childhood skin rash—it is a chronic, inflammatory, and intensely itchy condition that represents a complex interaction between genetics, immune dysfunction, and environmental triggers. Affecting up to 20% of children globally, it is the most common chronic skin disease in pediatrics. Characterized by a vicious “itch-scratch cycle,” eczema can significantly impact a child’s sleep, behavior, and quality of life, as well as the entire family’s well-being. Understanding its nature is the first step toward effective management and relief.
This guide provides a detailed, evidence-based overview of pediatric eczema, covering its causes, symptoms across ages, and a comprehensive, stepwise approach to daily management and flare-up control.
Part 1: Understanding the Root Causes: The “Atopic Triad”
Eczema is not a simple allergy or dry skin. It is part of the “atopic march,” a progression where children with eczema have a higher predisposition to later develop food allergies, asthma, and allergic rhinitis (hay fever). The exact cause is multifactorial:
Genetic Predisposition: A strong family history of eczema, asthma, or hay fever is common. Mutations in the filaggrin gene are a key discovery. Filaggrin is a protein crucial for forming the skin’s protective barrier. Its deficiency leads to “leaky” skin.
Immune System Dysregulation: An overactive immune response in the skin leads to inflammation, even in the absence of a true infection.
Skin Barrier Defect: This is the central problem. The skin of a child with eczema acts like a “brick wall” with missing mortar.
Healthy Skin: Tightly packed skin cells (bricks) held together by lipids like ceramides (mortar) retain moisture and keep irritants/allergens out.
Eczematous Skin: The barrier is compromised. Moisture escapes (transepidermal water loss), leading to dry, cracked skin. Irritants, allergens, and microbes can easily penetrate, triggering inflammation and itch.
Part 2: Recognizing Eczema: Symptoms by Age
Eczema’s appearance and common locations evolve as a child grows.
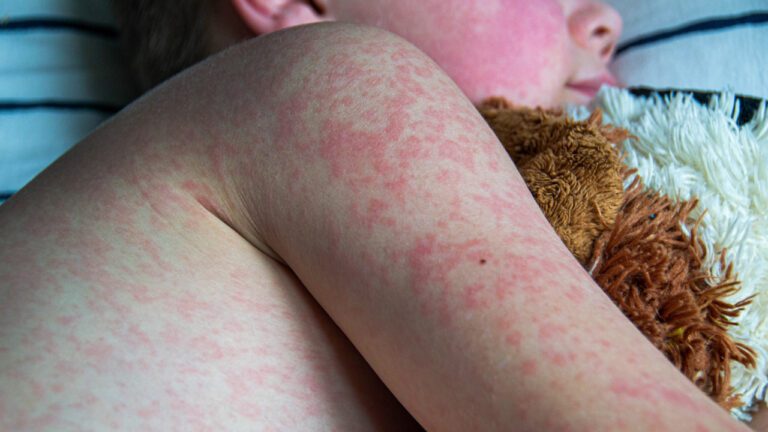
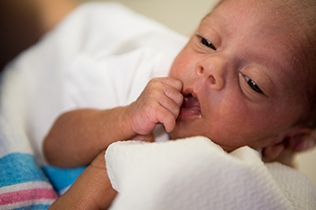
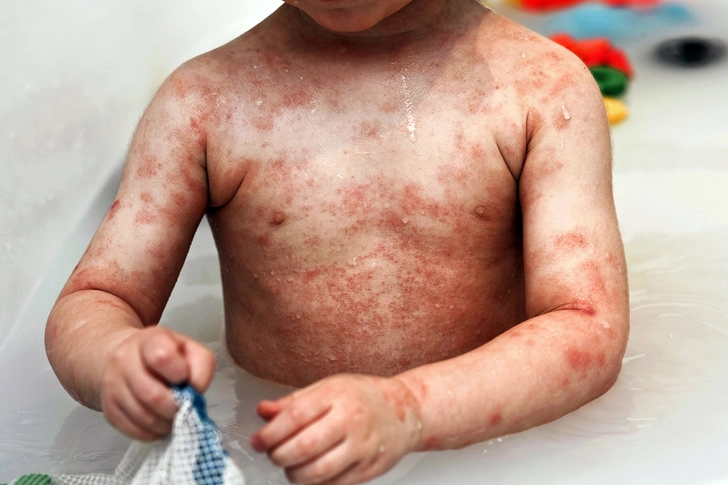
Infant Stage (2-6 months to 2 years):
Appearance: Red, weepy, crusted patches. Less commonly dry at this stage due to weeping.
Common Locations: Cheeks, scalp, forehead, and outer arms/legs. The diaper area is usually spared (protected by moisture).
Childhood Stage (Ages 2-12):
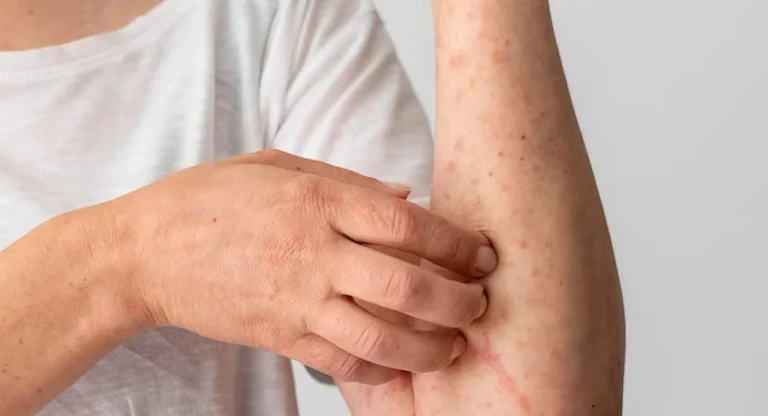
Appearance: Dry, scaly, thickened patches. Skin may look leathery (lichenification) from chronic scratching.
Common Locations: Creases of elbows and knees, wrists, ankles, neck, and around the eyes and mouth.
Adolescent/Adult Stage (Ages 12+):
Appearance: Chronic, dry, thickened plaques.
Common Locations: Hands, feet, flexural creases, face, and neck. Can be widespread.
Universal Hallmark: INTENSE ITCH (Pruritus). The itch is often worse at night, leading to sleep disruption. The itch-scratch cycle is self-perpetuating: itch leads to scratch, which damages the barrier further, causing more inflammation and more itch.
Part 3: Common Triggers: Knowing the Adversary
Identifying and minimizing triggers is a cornerstone of management.
Skin Irritants:
Soaps, bubble baths, and harsh detergents.
Saliva and drool (on cheeks/chin).
Rough, scratchy fabrics (wool, some synthetics).
Chlorine in pools.
Environmental Allergens (Inhalant): Dust mites, pet dander, pollen, mold.
Food Allergens: Can be a trigger in a subset of children (approx. 30%), typically those with moderate-to-severe eczema. Common culprits: milk, egg, peanut, soy, wheat. Do not eliminate foods without pediatrician/allergist guidance.
Climate: Low humidity (winter/dry climates), excessive heat/sweating.
Infections: Staphylococcus aureus bacteria often colonizes eczematous skin and can cause infected flares (yellow crust, pustules). Viral infections (like colds) can also trigger flares.
Stress: Emotional upset can exacerbate flares in older children.
Part 4: The Cornerstone of Management: Daily Skin Care (The “Baseline Therapy”)
Effective eczema control is 90% daily prevention and 10% treating flares. Think of it as a daily regimen for skin health.
1. Bathing: The “Soak and Seal” Method
Frequency: Short, lukewarm baths or showers once daily.
Cleanser: Use a gentle, fragrance-free, non-soap cleanser only on dirty areas. No bubble baths.
Soak: 5-10 minutes to hydrate skin.
Pat Dry: Gently pat skin with a towel, leaving it slightly damp.
2. Moisturizing (Emollients): The “Seal” – NON-NEGOTIABLE
Application: Apply a thick, fragrance-free ointment (like petroleum jelly) or cream within 3 minutes of bathing to trap moisture. Reapply at least 2-3 times daily, even on clear skin.
Product Choice: Ointments (greasiest) > Creams > Lotions (least effective). Creams like CeraVe, Cetaphil, Eucerin, or Vanicream are often ideal.
Part 5: Treating Flares: The Anti-Inflammatory Step
When flares occur (red, itchy patches), daily moisturizing is insufficient. This requires anti-inflammatory medication.
1. Topical Corticosteroids (TCS): The Mainstay Treatment.
Purpose: To quickly reduce inflammation and break the itch-scratch cycle.
Use: Applied once or twice daily to active red/itchy patches only, not to healthy skin. Used until the flare is completely clear (usually 3-14 days), then stopped.
Strength: Use the lowest effective potency prescribed by your doctor (e.g., hydrocortisone 1% for mild face/body, stronger for thick plaques).
Safety: Fear of TCS (“steroid phobia”) is common but unfounded when used correctly. Side effects (thinning skin) occur with inappropriate long-term, uninterrupted use on sensitive areas, not with proper flare management.
2. Topical Calcineurin Inhibitors (TCIs) – Non-Steroids
Medications: Tacrolimus (Protopic) & Pimecrolimus (Elidel).
Use: For sensitive areas (eyelids, face, neck) and for long-term maintenance to prevent flares. A steroid-sparing alternative.
3. Managing Infection:
Signs: Honey-colored crusts, pustules, worsening redness.
Treatment: May require prescription topical or oral antibiotics.
4. Breaking the Itch-Scratch Cycle:
Keep nails short and filed.
Wet wrap therapy: After applying medication/moisturizer, damp cotton clothing or gauze is applied, covered by a dry layer. Provides a physical barrier and deep hydration. Used for severe flares.
Antihistamines: Sedating types (like hydroxyzine or diphenhydramine) may be used short-term at bedtime primarily for their sedative effect to allow sleep, not primarily for itch relief during the day.
Part 6: Advanced Care & When to See a Specialist
For children with moderate-to-severe eczema uncontrolled by standard therapy:
Referral to a Pediatric Dermatologist or Allergist is recommended.
Advanced Therapies: May include biologic injections (Dupilumab/Dupixent, approved for children 6mo+), JAK inhibitors, or phototherapy.
See a Doctor If:
Eczema is severe, widespread, or not responding to over-the-counter care.
Signs of skin infection are present.
Itch is causing sleep deprivation or affecting school/behavior.
You need help identifying triggers or creating a management plan.
Part 7: The Emotional & Social Impact
Chronic itch and sleep disruption can lead to:
Irritability, mood swings, and difficulty concentrating.
Poor school performance.
Social embarrassment and withdrawal.
Family stress from care demands and sleep deprivation.
Supporting Your Child: Normalize the condition, advocate for them at school (e.g., allowing moisturizer at desk), and connect with support groups (National Eczema Association).
Conclusion: A Manageable Journey
While there is no definitive “cure” for eczema, it is a highly manageable condition. With a consistent, proactive daily regimen of gentle skin care and strategic use of anti-inflammatory medications during flares, most children achieve excellent control. Many will see significant improvement or outgrow the condition by adolescence. The goal is not perfect skin, but a comfortable, happy child who can sleep, play, and learn without being dominated by the itch. Through education, routine, and partnership with a healthcare provider, families can successfully navigate the challenges of eczema.
Other Posts