What Causes A Man’s Breasts To Grow
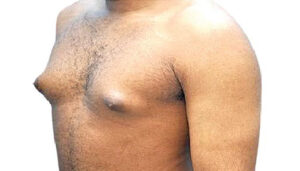
What Causes a Man’s Breasts to Grow? A Comprehensive Guide to Gynecomastia
Introduction: Demystifying Male Breast Enlargement
The development of noticeable breast tissue in men, a condition known as gynecomastia (pronounced guy-nuh-koh-MAST-ee-uh), is a common and often distressing phenomenon. Far from being a simple issue of weight gain, true gynecomastia involves a proliferation of glandular breast tissue beneath the nipple-areolar complex. It is distinct from pseudogynecomastia (or lipomastia), which is an accumulation of fat in the chest area without glandular growth, typically associated with obesity. Gynecomastia is fundamentally a hormonal imbalance—specifically, an increase in the ratio of estrogen (female hormones) to androgens (male hormones, like testosterone) in breast tissue. This guide provides a detailed, systematic exploration of the physiological, pharmacological, and pathological causes of male breast growth, offering clarity and a roadmap for evaluation.
Part 1: The Physiology of Gynecomastia – The Estrogen-Testosterone Seesaw
To understand gynecomastia, one must understand the hormonal environment of the male body.
Normal Male Physiology: All men produce both testosterone (the primary androgen) and estradiol (the primary estrogen), but testosterone levels are significantly higher. Testosterone inhibits breast tissue growth.
The Imbalance: Gynecomastia occurs when this ratio is disrupted in favor of estrogen. This can happen through three primary mechanisms:
Decreased Testosterone Production: As seen in hypogonadism (low testosterone) or aging.
Increased Estrogen Production: From tumors, exogenous sources, or increased peripheral conversion.
Androgen Receptor Blockade: Certain drugs prevent testosterone from acting on tissues, allowing estrogen’s effects to go unopposed.
The Breast Tissue Response: This hormonal shift stimulates the proliferation of ductal epithelium and stromal tissue in the male breast, leading to a firm, rubbery, often tender disc of tissue concentric to the nipple.
Part 2: The Lifespan of Gynecomastia – Physiologic (Normal) Causes
Not all gynecomastia is pathological. It is a normal finding at three key life stages due to natural hormonal fluctuations:
Newborns (“Neonatal Gynecomastia”): Maternal estrogens cross the placenta, causing transient breast tissue enlargement in up to 90% of newborns. It typically resolves within a few weeks.
Puberty (“Pubertal Gynecomastia”): Affects up to 70% of adolescent boys, usually between ages 12-15. It results from a temporary lag in testosterone production catching up to rising estrogen levels during the growth spurt. In over 90% of cases, it resolves spontaneously within 1-2 years as hormones stabilize.
Older Men (“Senile Gynecomastia”): In men over 50, the gradual, age-related decline in testosterone production, coupled with an increase in body fat (which aromatizes testosterone to estrogen), can lead to breast tissue growth. It is increasingly common with age.
Part 3: Pathological & Pharmacological Causes – The Medical Workup Triggers
When gynecomastia occurs outside the three physiologic windows, is painful, rapid in onset, or very pronounced, a medical investigation is warranted. The causes can be organized into several categories.
A. Medications (A Very Common Cause – 25% of Cases)
Many drugs induce gynecomastia by altering hormone metabolism or receptor activity.
Anti-androgens & Hormone Therapies: Flutamide, finasteride, dutasteride, ketoconazole, spironolactone, estrogen therapies (for prostate cancer).
Cardiovascular Drugs: Digoxin, calcium channel blockers (e.g., verapamil, nifedipine), ACE inhibitors, amiodarone.
Psychiatric/Neurologic Drugs: Typical and atypical antipsychotics (risperidone, haloperidol), tricyclic antidepressants, diazepam, phenytoin.
Recreational Drugs & Alcohol: Marijuana, heroin, methadone, amphetamines. Chronic heavy alcohol use can cause liver damage and hormonal disruption.
Others: Metronidazole, omeprazole, anti-retrovirals (for HIV), chemotherapy agents.
B. Underlying Health Conditions
Hypogonadism (Low Testosterone): Primary (testicular failure from Klinefelter syndrome, trauma, infection) or secondary (pituitary/hypothalamic disorders). Reduced testosterone leaves estrogen effects unopposed.
Hyperestrogenism:
Tumors: Rare, but testicular tumors (Leydig or Sertoli cell tumors, germ cell tumors) can secrete estrogens. Adrenal tumors can also produce estrogen precursors.
Liver Disease: Cirrhosis impairs the liver’s ability to metabolize estrogens, leading to elevated levels. Also increases sex hormone-binding globulin (SHBG), which binds testosterone, reducing free, active testosterone.
Hyperthyroidism: Increases SHBG, lowering free testosterone and altering the estrogen-testosterone ratio.
Chronic Kidney Disease: Alters hormone metabolism and can cause hyperprolactinemia, which can induce gynecomastia.
Malnutrition & Refeeding: Severe malnutrition suppresses gonadotropin production. Upon refeeding, a “rebound” in gonadotropins can cause a hormonal surge that stimulates breast tissue.
C. Herbal & Exogenous Products
Phytoestrogens: Plant-derived compounds with weak estrogenic activity, found in soy products, lavender oil, tea tree oil (topical use has been linked to prepubertal gynecomastia).
Anabolic-Androgenic Steroid (AAS) Abuse: A very common cause in bodybuilders. Exogenous androgens can be aromatized to estrogens. Furthermore, AAS use shuts down natural testosterone production, and when the cycle ends, a period of low testosterone/high estrogen can trigger significant gynecomastia (“post-cycle gyno”).
Part 4: Pseudogynecomastia vs. True Gynecomastia – A Critical Distinction
This is the first diagnostic step for a physician.
True Gynecomastia: Palpation reveals a firm, rubbery, disc-like mound of tissue that is concentric to and directly under the nipple-areolar complex. It may be tender. This is glandular proliferation.
Pseudogynecomastia (Lipomastia): Palpation reveals only soft, diffuse adipose (fat) tissue without a discrete firm mound. The chest contour is due to generalized fat accumulation, often associated with obesity.
Many men have a combination of both, especially if overweight.
Part 5: The Diagnostic Pathway – What to Expect at the Doctor
Evaluation begins with a detailed history and physical exam.
History: Onset, duration, tenderness, medication/drug use (prescription, OTC, herbal, recreational), symptoms of systemic disease (fatigue, weight loss, abdominal pain), symptoms of hypogonadism (low libido, erectile dysfunction, fatigue).
Physical Exam: Careful palpation of breasts, axillae, abdomen, and genitals (testicular size, masses). Assessment for stigmata of liver disease or hyperthyroidism.
Blood Tests:
Hormonal Panel: Testosterone (total and free), Estradiol, Luteinizing Hormone (LH), Follicle-Stimulating Hormone (FSH). This differentiates primary from secondary hypogonadism.
Liver and Kidney Function Tests: (AST, ALT, Bilirubin, Creatinine).
Thyroid Function Tests: (TSH).
Beta-HCG & AFP: Tumor markers for testicular cancer if a mass is palpated.
Imaging:
Breast Ultrasound: The imaging modality of choice to confirm glandular tissue and rule out rare male breast cancer (which is usually eccentric to the nipple, hard, and fixed).
Testicular Ultrasound: If a testicular mass is suspected or hormone levels are abnormal.
Biopsy: Rarely needed unless imaging suggests malignancy.
Part 6: Treatment and Management Strategies
Treatment is directed at the underlying cause. Physiologic gynecomastia often requires only reassurance and observation.
A. Medical Management (For Recent-Onset, Proliferative Phase)
If present for less than 12-18 months, tissue may still be responsive.
Discontinue Offending Agents: The first and most important step if a medication or supplement is the cause.
Medications:
Selective Estrogen Receptor Modulators (SERMs): Tamoxifen is the most effective, used off-label to block estrogen’s effect on breast tissue. Can reduce breast volume and pain.
Aromatase Inhibitors (e.g., Anastrozole): Block conversion of androgens to estrogens. Less consistently effective than SERMs for established gynecomastia.
B. Surgical Management
Indicated for long-standing gynecomastia (where fibrous tissue has replaced glandular tissue and is unresponsive to medication), severe psychological distress, or failed medical therapy.
Liposuction: Effective for removing the fatty (pseudogynecomastia) component.
Subcutaneous Mastectomy: Surgical excision of the glandular breast tissue through a periareolar incision. Often combined with liposuction and skin tightening for optimal contour. This is the definitive treatment.
Conclusion: A Manageable Condition with Clear Pathways
Gynecomastia is a multifaceted condition with roots in the delicate balance of sex hormones. While a source of significant embarrassment and anxiety for many men, it is crucial to understand that it is:
Very common across the lifespan.
Often benign and self-limiting (in puberty).
Frequently linked to reversible causes like medications or lifestyle factors.
Highly treatable once properly diagnosed.
The journey begins with a non-judgmental medical evaluation to distinguish true glandular growth from fat, identify the underlying driver, and formulate a targeted plan—whether that is watchful waiting, medical intervention, or surgical correction. By seeking professional guidance, men can address this condition effectively, restoring both physical comfort and confidence.
When to See a Doctor:
New, rapid, or painful breast enlargement.
A hard, fixed, or eccentric lump.
Nipple discharge (especially bloody).
Symptoms of systemic illness or hypogonadism.
Gynecomastia causing significant psychological distress.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician, endocrinologist, or urologist with any questions you may have regarding a medical condition.
Other Posts