Malnutrition In Older Adults

The Silent Epidemic: Understanding and Addressing Malnutrition in Older Adults
Introduction: An Invisible Crisis
Malnutrition in older adults represents one of the most significant yet underrecognized public health challenges of our aging population. Contrary to common perception, malnutrition isn’t solely about starvation or extreme thinness—it encompasses both undernutrition (insufficient nutrient intake) and overnutrition (excessive intake of calories with inadequate nutrients). Among older adults, a complex interplay of physiological, psychological, social, and economic factors creates a perfect storm for nutritional deficiencies that quietly undermine health, independence, and quality of life.
This comprehensive examination explores the multifaceted nature of geriatric malnutrition, its devastating consequences, and evidence-based solutions for prevention and intervention.
Section 1: The Scope and Scale of the Problem
Prevalence Statistics: More Common Than You Think
Community-Dwelling Older Adults: 5-10% are malnourished, with an additional 30-60% at risk
Hospitalized Elderly: 20-50% experience malnutrition upon admission
Long-Term Care Facilities: 30-50% of residents are malnourished
After Hospitalization: 65% of older adults experience nutritional decline post-discharge
The Economic Burden
Malnutrition in older adults carries staggering costs:
Healthcare Expenses: Malnourished seniors incur healthcare costs 300% higher than well-nourished peers
Extended Hospital Stays: Average 2-3 days longer with associated costs of $2,000-$3,000 per day
Institutionalization: Malnutrition increases risk of nursing home admission by 40%
Total U.S. Burden: Estimated at $51.3 billion annually in direct medical costs
Section 2: The Complex Web of Causes
Malnutrition in older adults rarely stems from a single cause but emerges from interconnected factors:
Physiological Changes (The “Anorexia of Aging”)
Sensory Decline:
Taste buds diminish by 50% by age 60, reducing pleasure in eating
Smell impairment affects 75% of those over 80, diminishing food enjoyment
Vision problems make food preparation and shopping difficult
Gastrointestinal Alterations:
Reduced stomach acid affects protein digestion and B12 absorption
Slowed gastric emptying increases satiety
Altered gut microbiota affects nutrient absorption
Metabolic and Hormonal Shifts:
Decreased leptin sensitivity disrupts appetite regulation
Increased cholecystokinin (satiety hormone) reduces hunger
Reduced growth hormone and testosterone decrease muscle synthesis
Dental and Oral Health:
20% of older adults have no natural teeth
50% have untreated tooth decay
Ill-fitting dentures affect chewing ability
Medical Factors
Chronic Diseases: COPD, heart failure, cancer, dementia, and kidney disease increase metabolic demands while decreasing appetite
Polypharmacy: The average older adult takes 4-5 prescription medications, many with nutritional side effects:
Diuretics: Deplete potassium and magnesium
Metformin: Reduces B12 absorption
SSRIs: Alter taste perception
Chemotherapy: Causes nausea and mouth sores
Acute Illness and Inflammation: Hospitalization triggers catabolism (muscle breakdown) that continues post-discharge
Psychological and Cognitive Factors
Depression: Affects 15-20% of community-dwelling older adults, strongly linked to appetite loss
Dementia: 30-40% of Alzheimer’s patients experience significant weight loss due to:
Forgetting to eat
Inability to recognize food
Swallowing difficulties (dysphagia) in later stages
Social Isolation and Loneliness: Eating alone reduces food intake by 30-50%
Grief and Bereavement: Loss of spouse often leads to nutritional decline
Socioeconomic Barriers
Financial Constraints: 15% of older Americans live below the poverty line; many face “heat or eat” dilemmas
Food Deserts: 30% of older adults in rural areas lack access to grocery stores
Transportation Limitations: 20% of non-drivers report difficulty obtaining food
Functional Limitations: 25% of those over 65 have difficulty with shopping or meal preparation
Section 3: Identifying Malnutrition: Beyond the Scale
Screening Tools
Mini Nutritional Assessment (MNA®): Gold standard with 96% sensitivity
Malnutrition Universal Screening Tool (MUST): Widely used in clinical settings
SCREEN II: Validated for community settings
Clinical Signs Often Missed
Unexplained Weight Loss: >5% in 30 days or >10% in 6 months
Changes in Fit: Rings slipping off, dentures becoming loose
Skin and Hair Changes:
Dry, flaky skin with poor turgor
Hair thinning or loss
Easy bruising
Oral Indicators:
Angular cheilitis (cracks at mouth corners)
Bleeding gums
Smooth, red tongue (B vitamin deficiencies)
Functional Decline:
Reduced handgrip strength
Slow walking speed
Difficulty rising from chair
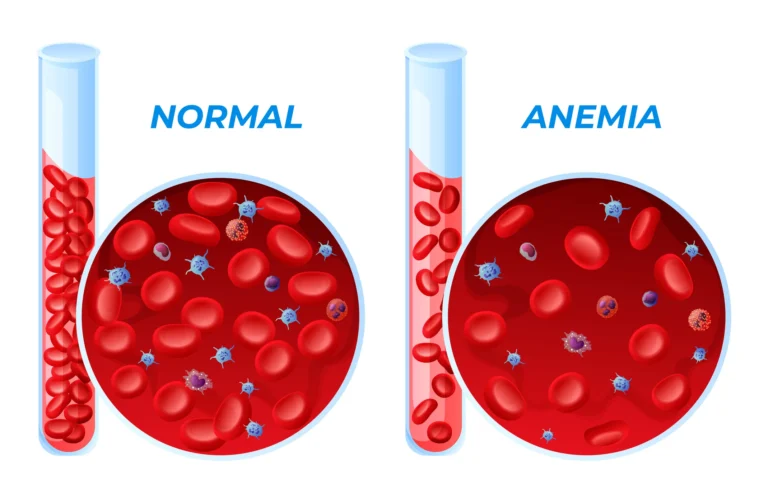
Laboratory Markers:
Albumin <3.5 g/dL (though affected by inflammation)
Prealbumin <15 mg/dL
Vitamin D <20 ng/mL (affects 50% of older adults)
Vitamin B12 <200 pg/mL (deficient in 20%)
The Sarcopenia-Malnutrition Connection
Sarcopenia (age-related muscle loss) accelerates with poor nutrition:
After age 50: Muscle mass declines 1-2% annually
Strength declines 1.5-5% yearly
By age 80: 40% of muscle mass may be lost
Malnutrition accelerates this process, creating frailty
Section 4: The Devastating Consequences of Geriatric Malnutrition
Physical Health Impacts
Immune Dysfunction:
3x increased infection risk
Poor vaccine response
Delayed wound healing
Musculoskeletal Decline:
2-3x increased falls risk
3-4x increased fracture risk
70% longer recovery from hip fractures
Organ System Effects:
Cardiac muscle wasting increases heart failure risk
Respiratory muscle weakness raises pneumonia risk
Impaired thermoregulation increases hypothermia risk
Increased Mortality:
Malnourished hospitalized elders have 4-6x higher mortality
Even mild malnutrition doubles mortality risk over 3 years
Cognitive and Psychological Effects
Accelerated Cognitive Decline: Nutritional deficiencies (especially B vitamins) speed dementia progression
Increased Depression: Malnutrition and depression form a vicious cycle
Reduced Neurotransmitter Production: Protein deficiency limits dopamine and serotonin synthesis
Functional and Social Consequences
Loss of Independence: Malnutrition precedes 50% of nursing home admissions
Reduced Quality of Life: Malnourished elders report significantly lower life satisfaction
Healthcare Utilization: Increased hospital readmissions, longer stays, more complications
Section 5: Evidence-Based Interventions and Solutions
Nutritional Strategies
Protein Optimization:
Need: 1.0-1.2 g/kg body weight daily (higher than younger adults)
Strategy: 25-30g protein per meal, emphasizing leucine-rich sources (whey, eggs, fish)
Timing: Protein evenly distributed throughout day maximizes muscle synthesis
Calorie Enhancement:
Small, frequent meals (6-8 daily) better tolerated than 3 large meals
Nutrient-dense foods: eggs, avocado, nut butters, olive oil
Fortified foods: protein powders added to soups, cereals, smoothies
Micronutrient Focus:
Vitamin D: 800-2000 IU daily with calcium (600-800 mg)
Vitamin B12: 500-1000 mcg supplementation often needed due to reduced absorption
Zinc and Magnesium: Common deficiencies affecting immunity and muscle function
Oral Nutritional Supplements (ONS):
Evidence: Reduce mortality by 24% and complications by 18% in malnourished elders
Effective Use: Between meals, not with meals; varied flavors to prevent taste fatigue
Cost-Effectiveness: Every $1 spent on ONS saves $52 in healthcare costs
Environmental and Behavioral Interventions
Mealtime Environment:
Social dining increases intake by 30-50%
Pleasant atmosphere with adequate lighting
Noise reduction to improve focus on eating
Family-style serving encourages second helpings
Food Modification:
For Chewing Difficulties: Moist, soft foods; finely chopped or pureed
For Swallowing Issues: Texture-modified diets with proper thickeners
For Taste Alterations: Enhanced flavors with herbs, spices, citrus
Feeding Assistance:
Proper positioning: upright at 90°, chin slightly tucked
Adaptive utensils for arthritis
Verbal encouragement without rushing
Recognition of fatigue: smaller portions with seconds offered
System-Level Solutions
Screening Implementation:
Universal screening at primary care visits
Hospital admission and discharge protocols
Community program eligibility assessments
Interprofessional Collaboration:
Registered Dietitian Nutritionists: Lead nutritional care
Speech Language Pathologists: Address swallowing disorders
Dentists/Oral Hygienists: Maintain oral health
Occupational Therapists: Adaptive equipment and strategies
Social Workers: Address socioeconomic barriers
Community-Based Programs:
Meals on Wheels: Reduces food insecurity by 70% and loneliness by 50%
Congregate Dining: Provides social connection with nutrition
Food Pharmacies: Prescription-based food assistance
Transportation Services: Grocery shopping assistance
Caregiver Education and Support:
Nutrition education tailored to dementia care
Respite services to prevent burnout
Support groups for problem-solving
Section 6: Special Populations and Considerations
Dementia-Related Malnutrition
Environmental Modifications:
Contrasting plates (dark plate, light food) improve visual recognition
Finger foods maintain independence in later stages
One food at a time reduces confusion
Behavioral Approaches:
Music during meals decreases agitation
Modeling eating behavior encourages imitation
Calm, consistent routines
Hospitalized Older Adults
Protected Mealtimes: No interruptions during meals
Feeding Assistance: Trained volunteers or staff
Menu Flexibility: Options available at all hours
Discharge Planning: Nutritional status included in transition protocols
Cultural and Ethnic Considerations
Respect Food Preferences: Traditional foods increase acceptance
Religious Observances: Accommodate dietary restrictions
Language-Appropriate Education: Overcome communication barriers
Section 7: The Future of Geriatric Nutrition
Emerging Innovations
Personalized Nutrition: Genetic testing to tailor dietary recommendations
Digital Solutions:
Smart plates that monitor intake
Apps for meal tracking and reminders
Tele-nutrition for rural access
Functional Foods: Specifically designed for aging physiology
Pharmaconutrition: Targeted nutrient combinations to address specific conditions
Policy Initiatives Needed
Medicare Expansion: Coverage for medical nutrition therapy
Healthcare Integration: Nutritional care as quality measure in value-based care
Research Funding: Increased NIH allocation for aging and nutrition studies
Workforce Development: More geriatric-trained dietitians and culinary professionals
Conclusion: A Call to Action
Malnutrition in older adults is neither inevitable nor acceptable. It represents a systemic failure to recognize changing nutritional needs across the lifespan and to implement known solutions. Addressing this crisis requires a paradigm shift from viewing feeding as mere sustenance to understanding nutrition as fundamental medical therapy.
The most effective approach combines:
Universal awareness among healthcare providers, caregivers, and older adults themselves
Routine screening across all settings
Timely intervention with evidence-based strategies
Multidisciplinary collaboration that addresses root causes
Policy support that removes barriers to adequate nutrition
As global populations age, our collective response to geriatric malnutrition will determine whether added years of life become years of vitality or years of decline. The solutions exist; what’s needed is the will to implement them systematically and compassionately.
Every older adult deserves the dignity of adequate nourishment—not merely to extend life, but to enhance its quality, preserve independence, and honor the accumulated wisdom of our elders with the nutritional support they need to thrive in their later years.
“The measure of a society is how it treats its most vulnerable members.” This ancient wisdom finds particular relevance in how we address the nutritional needs of our aging population. Malnutrition is not merely a medical condition but a reflection of our communal values. By ensuring our elders are well-nourished, we nourish the very soul of our society.
Other Posts